jod basedow syndrome from iodine load in hyperthyroidism
- related: hyperthyroidism and thyroiditis
- tags: #literature #endocrine
The patient developed fever, altered mental status, rapid atrial fibrillation, and heart failure after coronary angiography, a constellation of findings that should suggest the possibility of thyroid storm, a diagnosis that was confirmed by blood tests showing a low thyroid-stimulating hormone level and high free thyroxine (T4) level. Thyroid storm usually occurs in the setting of previous hyperthyroidism, but that hyperthyroidism may not have been previously diagnosed. Thyroid storm in a patient with subclinical hyperthyroidism can be precipitated by administration of iodinated contrast material (Jod-Basedow syndrome), as it was in this case.
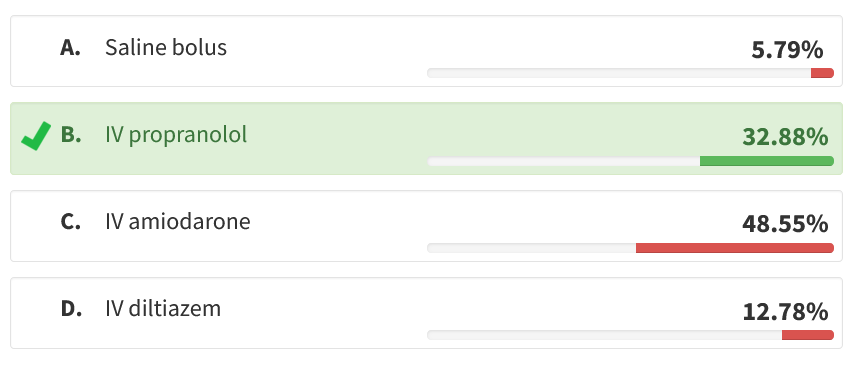
The pathophysiology of thyroid storm probably results from a combination of effects of thyroid hormone and sympathetic activation. As such, tachycardia is usually treated with nonselective β-blockers. In the setting of heart failure, β-blockers should be given with some caution, but rate control often increases BP and improves cardiac output in this setting. Propranolol is the classic β-blocker employed in thyroid storm because, in addition to inhibiting the peripheral effects of hyperthyroidism, it also inhibits conversion of thyroxine (T4) to triiodothyronine (T3), but esmolol is an alternative, and nonselective β-blockers may be useful as well (choice B is correct). The patient was mildly hypotensive with a low pulse pressure, but fluid administration is not helpful in the presence of frank heart failure (choice A is incorrect). Diltiazem can slow heart rate but has negative inotropic effects and does not address the underlying hypersympathetic state (choice D is incorrect). Amiodarone contains iodine and is contraindicated in patients with thyroid disease (choice C is incorrect).
Other therapy for thyroid storm includes inhibition of new thyroid hormone synthesis, which is usually done with propylthiouracil because this also decreases conversion of T4 to T3, and glucocorticoids, which decrease conversion of T4 to T3 and also may modulate autoimmunity and correct relative adrenal insufficiency. Exogenous iodine is often given after a drug to inhibit hormone synthesis is on board because this inhibits release of preformed hormone from the thyroid gland (Wolff-Chaikoff effect), but it should be noted that the Jod-Basedow effect represents the opposite of this response. Bile acid sequestrants may reduce thyroid hormone levels by interfering with enterohepatic recirculation and enhancing clearance. Lithium can also be used acutely to block release of thyroid hormone, but renal and neurologic effects limit its benefits. Definitive therapy for hyperthyroidism involves radioactive iodine or thyroidectomy.123
A 66-year-old woman presents with left arm discomfort and shortness of breath. Her BP is 110/70 mm Hg, heart rate is 70/min, and respirations are 12/min. Physical examination is normal. The presenting ECG shows lateral ST depression, and the cardiac troponin level is elevated, so she is taken to cardiac catheterization, where a drug-eluting stent is placed. Left ventricular function is normal by ventriculography. The next morning, she presents with tachycardia and shortness of breath and is noted to be in atrial fibrillation with a rate between 110-130/min. She is taken back to the catheterization laboratory, where the stent is shown to be patent. Following the repeat catheterization, she is agitated and confused. Her BP is 100/75 mm Hg, heart rate is 150-160/min, respirations are 36/min, and temperature is 39.6°C. She has bilateral crackles on lung exam, with a rapid irregular heart rhythm with an S3 gallop. The abdomen is mildly tender, and there is bilateral pedal edema.
Which of the following is most likely to produce clinical improvement now?
Links to this note
Footnotes
-
Chiha M, Samarasinghe S, Kabaker AS. Thyroid storm: an updated review. J Intensive Care Med. 2015;30(3):131-140. PubMed ↩
-
El-Shirbiny AM, Stavrou SS, Dnistrian A, et al. Jod-Basedow syndrome following oral iodine and radioiodinated-antibody administration. J Nucl Med. 1997;38(11):1816-1817. PubMed ↩