evacuation of IPH has outcome improvement
- related: Neurology
- tags: #literature #icu #neuro
The treatment of intraparenchymal hemorrhage has been limited for decades to management of acute hypertension, reversal of anticoagulation (not an issue in this patient), and supportive care. Previous studies investigating hemorrhage evacuation have failed to show benefit, partly because of the destructive nature of open intracranial surgery and the methodological problems in the studies. Subset analysis of a large multinational randomized trial in the 1990s showed a trend toward benefit by using minimally invasive techniques of hemorrhage evacuation. A trial of catheter placement into the hemorrhage followed by instillation of tissue plasminogen activator (MISTIE III) failed to meet the prespecified end points but showed that patients with the most complete evacuations improved more than did those with less evacuation. The ENRICH trial showed that minimally invasive evacuation of lobar hemorrhages (between the basal ganglia and cortex in the subcortical white matter) and intraparenchymal hemorrhages improves outcome in patients (choice D is correct). Of note, cerebellar hemorrhages are often treated surgically with either decompressive suboccipital craniotomy or hemorrhage evacuation, and these were excluded from this trial.
The placement of an external ventricular drain is indicated in patients with hydrocephalus either from intraventricular hemorrhage or from compression of the ventricle. There is no evidence that this patient is experiencing either of these problems (choice A is incorrect). Intracranial pressure monitors are used to determine whether elevated intracranial pressure needs to be treated. As this is a monitoring device, it lacks the effect of hemorrhage evacuation, although placement later in the course of the hospital stay is indicated if increased intracranial pressure is suspected (choice B is incorrect). A trial of enforced normothermia (the INTREPID trial) in patients with acute ischemic strokes, subarachnoid hemorrhage, and intraparenchymal hemorrhage was halted early owing to futility (choice C is incorrect). Methodological problems with the power calculation and poor enrollment in the INTREPID study suggest that temperature modulation may still be a reasonable treatment for intraparenchymal hemorrhage.12
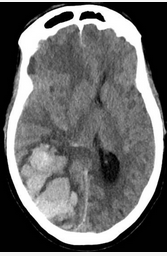
A 45-year-old woman with a medical history of hypertension presents with the acute onset of loss of consciousness and left hemiparesis. She undergoes intubation in the field for poor airway protection. A CT scan obtained at admission is shown (Figure 1). The CT scan showed no extension of the hemorrhage into the ventricular system. On examination, she has a BP of 190/100 mm Hg, heart rate of 70/min, respiratory rate of 12/min with pressure-control ventilation, and a temperature of 37.9 °C.
After treatment of her hypertension, which of the following interventions is most likely to improve her outcome?
Links to this note
Footnotes
-
Hanley DF, Thompson RE, Rosenblum M, et al; MISTIE III Investigators. Efficacy and safety of minimally invasive surgery with thrombolysis in intracerebral haemorrhage evacuation (MISTIE III): a randomised, controlled, open-label, blinded endpoint phase 3 trial. Lancet. 2019;393(10175):1021-1032. PubMed ↩